How Insulin Resistance Links PCOS and Fasting
Insulin resistance plays a major role in Polycystic Ovary Syndrome (PCOS), affecting up to 75% of women with this condition. It leads to excess insulin production, which drives higher androgen levels, worsening symptoms like irregular periods, acne, and fertility issues. Fasting, particularly intermittent fasting (like 16:8 or time-restricted eating), can help by lowering insulin levels, improving insulin sensitivity, and balancing hormones.
Key takeaways:
- PCOS and Insulin Resistance: Up to 80% of women with PCOS experience insulin resistance, which worsens hormonal imbalances and increases the risk of Type 2 diabetes.
- Fasting Benefits: Fasting reduces insulin levels, encourages fat burning, and supports hormone regulation, helping with weight loss, menstrual regularity, and fertility.
- Research Insights: Studies show fasting can lower fasting insulin, reduce testosterone, and improve ovulation, but results vary, and more research is needed.
- Personalized Care Matters: Tailored fasting plans, combined with medical oversight, are essential to address individual PCOS symptoms and risks.
Fasting offers a promising approach to managing PCOS, but expert guidance ensures safety and effectiveness.
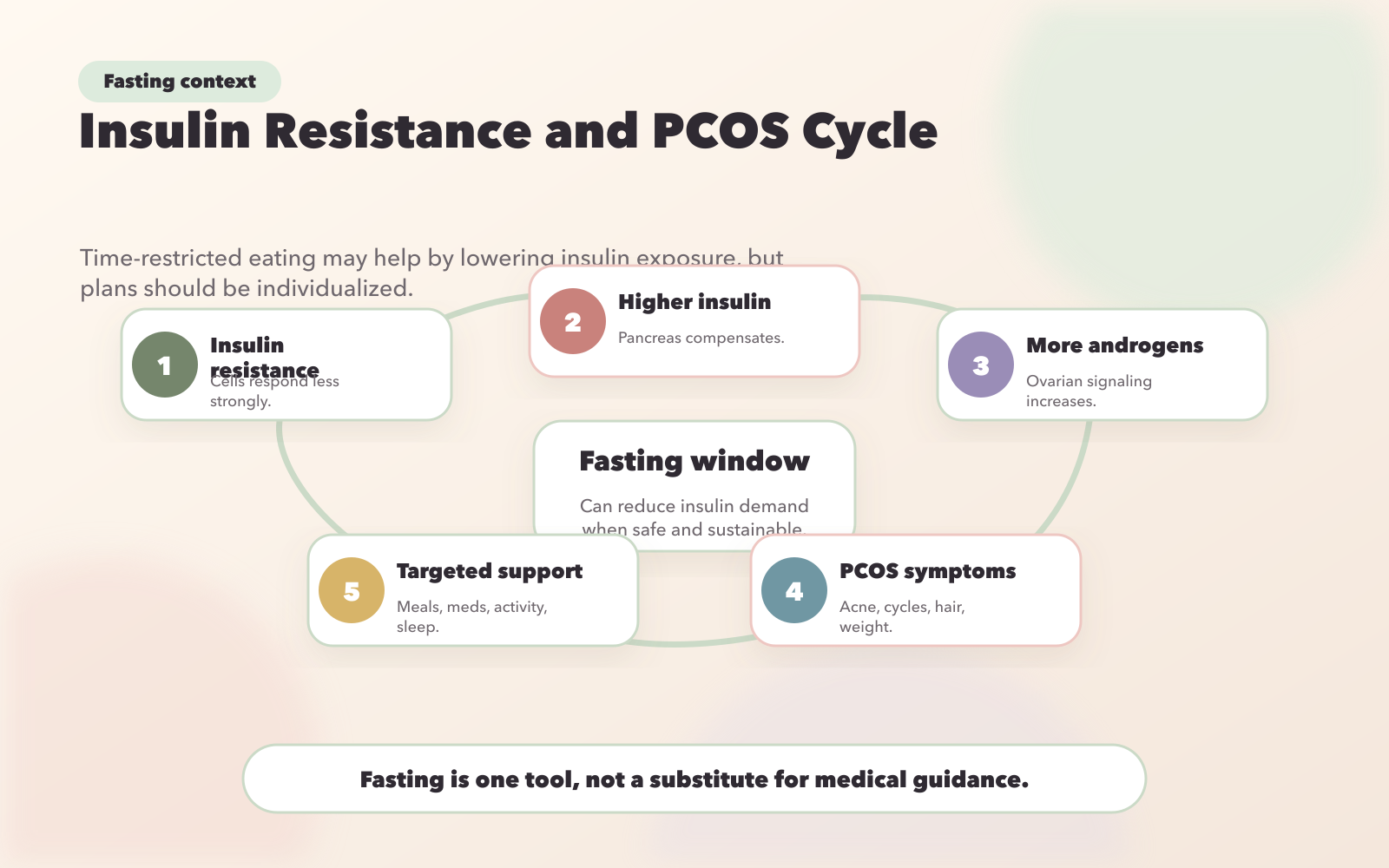
The Insulin Resistance and PCOS Vicious Cycle: How Fasting Breaks the Chain
Insulin Resistance and PCOS: How They're Connected
What Is Insulin Resistance?
Insulin resistance happens when your muscle, fat, and liver cells don’t respond well to insulin - a hormone that helps glucose enter cells to be used for energy. To make up for this, the pancreas produces more insulin, leading to a condition called hyperinsulinemia, which plays a major role in PCOS symptoms.
Between 65% and 70% of women with PCOS have insulin resistance, and those numbers climb to 70–80% in women who are obese. Even women with PCOS who aren’t overweight often show signs of insulin resistance, although usually to a lesser degree. Additionally, up to 85% of women with classic PCOS - marked by anovulation and high androgen levels - experience hyperinsulinemia.
These statistics highlight how common insulin resistance is in PCOS and why it significantly impacts hormonal imbalances.
How Insulin Resistance Worsens PCOS Symptoms
Elevated insulin levels directly encourage the ovaries to produce more androgens, such as testosterone. Acting as a co-gonadotropin, insulin teams up with other hormones to stimulate ovarian theca cells to ramp up male hormone production. It also boosts the activity of cytochrome P450c17α, an enzyme critical for androgen synthesis.
On top of that, hyperinsulinemia reduces the liver's production of Sex Hormone Binding Globulin (SHBG), which leads to higher levels of free testosterone circulating in the blood. This hormonal imbalance can trigger symptoms like stubborn acne, excessive facial and body hair (hirsutism), and thinning scalp hair. Together, increased insulin and androgen levels throw off the balance of reproductive hormones, resulting in irregular periods and problems with ovulation.
"Insulin resistance is a unifying feature [of PCOS]. Reciprocal interactions among androgen excess, hyperinsulinemia, and reduced hepatic sex hormone-binding globulin production create a self‑sustaining 'vicious cycle' that exacerbates PCOS manifestations." - Nature
This cycle not only raises androgen levels but also encourages abdominal fat gain, which increases inflammation. This inflammation further damages insulin receptors, worsening insulin resistance. Women with PCOS are therefore four to nine times more likely to develop diabetes than those without PCOS, with over 50% being diagnosed with Type 2 diabetes by the time they reach 40.
How Fasting Improves Insulin Sensitivity
What Happens to Your Metabolism During Fasting
After about 12 hours without food, your liver runs out of stored glycogen, forcing your body to switch gears. Instead of relying on glucose for energy, it begins burning stored fat, producing ketones as an alternative fuel source. This process is known as "metabolic switching" - a shift that has profound effects on your body.
One of the key benefits of this switch is reduced insulin release. With less insulin circulating, your body's receptors have a chance to reset and become more responsive.
"A period of daily fasting depletes liver glycogen stores and switches energy sources to fatty acid and ketones. This bioenergetic challenge activates signalling pathways that strengthen mitochondrial function and stress resistance." - R Floyd, Department of Endocrinology, Tallaght University Hospital
Fasting also triggers autophagy, a natural cellular cleanup process. During autophagy, cells break down and recycle damaged components while reinforcing their mitochondria - the energy-producing structures that often underperform in insulin-resistant conditions. This cellular renewal plays a direct role in improving how well your body responds to insulin.
Together, these metabolic shifts not only lower insulin levels but also enhance insulin sensitivity, setting the stage for better overall metabolic health.
Fasting Benefits for Insulin Resistance
For women dealing with PCOS, fasting can be a game-changer. Research on the 16:8 fasting method - 16 hours of fasting followed by an 8-hour eating window - revealed significant improvements in insulin resistance markers. Over just five weeks, participants saw reductions in fasting insulin levels, HOMA-IR scores (a key measure of insulin resistance), and body fat mass. On average, they lost 2.9 lbs (1.3 kg) and reduced visceral fat, which is the harmful abdominal fat linked to inflammation and worsening insulin resistance.
Lower insulin levels during fasting also help balance hormones. By decreasing ovarian androgen production and increasing the liver's output of SHBG (sex hormone-binding globulin), fasting can address hormonal imbalances that drive PCOS symptoms like acne, unwanted hair growth, and irregular periods. These changes directly target the root causes of PCOS, offering relief for many of its challenging symptoms.
How Fasting Affects Hormones and Weight in PCOS
Lowering Androgen Levels and Improving Ovulation
Fasting doesn’t just improve insulin sensitivity - it also directly influences hormone levels. By lowering insulin levels, fasting reduces ovarian stimulation and the production of excess testosterone. A clinical trial conducted in January 2021 observed 15 women with anovulatory PCOS who followed an 8-hour eating window for five weeks. The results were striking: total testosterone and the Free Androgen Index dropped significantly, while levels of Sex Hormone-Binding Globulin (SHBG) increased. Even more compelling, 73.3% of the participants resumed normal menstrual cycles.
The rise in SHBG is particularly important because it binds to testosterone, reducing the amount of active testosterone in the body. These hormonal adjustments play a key role in promoting regular ovulation for women managing PCOS.
Weight Loss and Metabolic Health
Fasting also brings changes to body composition, which is critical for managing PCOS. A study at Al-Mafraq Hospital in Jordan examined 86 overweight women with PCOS who followed an 18-hour fasting protocol. On average, these participants lost 20.3 lbs (9.2 kg), compared to just 5.3 lbs (2.4 kg) in the non-fasting group. Additionally, they reduced visceral fat by 5.1 lbs (2.3 kg) and gained 4.9 lbs (2.2 kg) of muscle.
This reduction in visceral fat is especially beneficial, as it lowers inflammation and enhances insulin sensitivity. Research shows that even a modest 5% weight loss can regulate menstrual cycles and boost fertility. These improvements directly address the metabolic challenges that are often part of PCOS.
What Research Shows About Fasting and PCOS
Current Research Findings on Fasting for PCOS
Recent studies suggest fasting may help manage PCOS, though the results aren't definitive yet. For example, a 2021 study conducted at Shengjing Hospital of China Medical University observed 15 women with anovulatory PCOS who followed an 8-hour time-restricted feeding schedule (from 8:00 AM to 4:00 PM) for five weeks. The study reported reductions in fasting insulin levels and improvements in menstrual cycle regularity, with 11 out of 15 participants experiencing better patterns. Researchers noted, "the diet of TRF may be beneficial to anovulatory PCOS on weight loss especially reducing body fat, improving menstruation, hyperandrogenemia, insulin resistance and chronic inflammation".
Another study in Jordan, conducted between November 2022 and July 2023, examined the effects of 18-hour fasting three times a week. Participants in the fasting group lost an average of 20.3 lbs (9.2 kg), while the control group lost only 5.3 lbs (2.4 kg). However, a 2025 meta-analysis found no significant changes in fasting glucose or HOMA-IR levels. These mixed results highlight the complexity of fasting's effects on PCOS and the need for further investigation.
Gaps in Current Research
Despite these promising findings, the research landscape is far from complete. Many studies are limited by small sample sizes, short durations (typically 4–8 weeks), and reliance on participants' self-reported adherence to fasting protocols. A key question remains: are the observed benefits due to the timing of meals, or are they simply the result of reduced calorie intake overall?.
Experts emphasize the need for more robust studies, particularly large-scale, randomized controlled trials, to develop clear guidelines for using fasting as a potential strategy for managing PCOS. Until then, personalized medical advice is essential for anyone considering fasting as part of their PCOS management plan.
sbb-itb-6dba428
Getting Medical Guidance for PCOS and Fasting
Why Personalized Care Matters
PCOS presents itself in four distinct phenotypes (A, B, C, D), each with varying levels of insulin resistance and metabolic risks. A study involving 200 women revealed significant differences between these phenotypes: 69.57% of women with Phenotype A (the most severe type) experienced insulin resistance, compared to just 26.09% of those with Phenotype C. The study also highlighted variations in HOMA-IR values - a key measure of insulin resistance - ranging from 2.05 in Phenotype C to 3.59 in Phenotype A.
These differences underline the need for tailored fasting protocols. For instance, individuals with classic PCOS often face challenges like hyperinsulinemia, and common treatments such as oral contraceptives can further complicate insulin sensitivity. As noted in Medical Hypotheses:
"The studies in humans should be performed under careful medical control, checking in particular basal and under-treatment glycaemia, plasmatic insulin and IGF-1".
Additionally, women with PCOS face heightened long-term health risks. A healthcare provider can help you navigate these complexities by monitoring important biomarkers, such as baseline Human Growth Hormone (HGH), and customizing your fasting schedule based on your metabolic profile and any medications you may be taking, like Metformin. This level of personalized oversight is essential for safely incorporating fasting into a PCOS management plan. The intricate nature of PCOS makes specialized medical support indispensable.
How Oana Health Helps Women with PCOS

To address these challenges, Oana Health offers telehealth services tailored specifically for women managing PCOS, insulin resistance, and hormonal imbalances. Rather than relying on generic recommendations, their licensed medical professionals develop personalized treatment plans that consider your unique symptoms, health history, and metabolic markers.
Their treatments target the root causes of PCOS symptoms using science-backed approaches delivered directly to your home. Available options include Oral Metformin ER ($22/month) for insulin resistance, a Metformin & Spironolactone combination ($32/month) for hormonal balance, and Oral GLP-1 & Metformin ($199/month) for more advanced management. They also offer targeted solutions like Oral Minoxidil ($25/month) and Eflornithine 12% ($69/month) for addressing hair-related symptoms.
Getting started is simple: an online consultation allows a licensed provider to review your medical history and create a personalized prescription plan - all from the comfort of your home. This convenience is particularly beneficial for women integrating fasting into their PCOS management, as it ensures consistent medical oversight to keep your approach safe and effective as your body adapts to dietary changes.
Intermittent Fasting and PCOS
Conclusion
High insulin levels in PCOS create a challenging cycle: they increase androgen production and abdominal fat, which worsens insulin resistance and raises the risk of Type 2 diabetes.
Intermittent fasting offers a way to interrupt this cycle. Studies show that time-restricted eating can lower fasting insulin levels, improve HOMA-IR scores, and reduce total testosterone. For instance, a five-week study revealed that 73.3% of women with anovulatory PCOS saw improvements in menstrual regularity. Additionally, the metabolic changes triggered by fasting - such as transitioning to ketogenesis and burning fatty acids - may help reduce visceral fat and enhance insulin sensitivity. These findings highlight the potential of fasting as part of a broader strategy, but they also underline the importance of individualized medical care.
PCOS manifests in various ways, with insulin resistance levels differing greatly among individuals. This diversity makes personalized treatment essential. Addressing the insulin-PCOS cycle effectively requires tailored fasting protocols combined with expert medical oversight.
To meet these needs, Oana Health offers specialized care designed to navigate the complexities of PCOS safely. Their licensed professionals develop customized treatment plans, which may include options like Oral Metformin ER ($22/month) for managing insulin resistance, alongside combination therapies for broader hormonal balance. All therapies are delivered directly to your home with free shipping.
Successfully managing PCOS involves more than one-size-fits-all advice. It requires a science-driven, personalized approach that takes into account your unique hormonal profile, medical history, and lifestyle.
FAQs
How can fasting help improve insulin sensitivity in women with PCOS?
Fasting methods, like time-restricted eating (such as limiting meals to an 8-hour window), can play a key role in improving insulin sensitivity for women with PCOS. By shortening the period during which insulin circulates in the body, fasting gives insulin receptors a chance to reset and function more effectively. This improved receptor activity helps regulate blood sugar levels more efficiently and can also reduce inflammation.
Beyond blood sugar management, fasting supports a healthier hormonal balance, which may help ease common PCOS symptoms such as weight gain, acne, and irregular menstrual cycles. When incorporated into a tailored treatment plan, fasting could provide lasting benefits for addressing insulin resistance and other challenges linked to PCOS.
What are the risks of fasting for women with PCOS?
Fasting has been shown to lower insulin levels, which can be beneficial for some. However, for women managing PCOS, it’s not without potential challenges. Prolonged fasting might lead to blood sugar swings, which can trigger fatigue, mood changes, or sudden cravings. It could also interfere with reproductive hormones, possibly causing irregular periods or impacting ovulation.
Pairing fasting with low-calorie diets might further complicate things, increasing the risk of nutrient deficiencies or even muscle loss. Since every individual reacts differently, women with PCOS should approach fasting cautiously and ideally under medical guidance. Oana Health provides personalized telehealth services designed to track insulin resistance, menstrual health, and overall well-being, ensuring that symptom management is both safe and effective.
Is fasting effective for managing all types of PCOS, or does it work better for certain types?
Fasting, whether through intermittent fasting or time-restricted eating, has been shown to support better insulin sensitivity, stabilize glucose levels, and address hormonal imbalances often linked to polycystic ovary syndrome (PCOS). Still, its effectiveness can depend on the specific type of PCOS a person has.
For women with insulin-resistant PCOS - often referred to as the "classic" or "hyperandrogenic-insulin resistant" type - fasting tends to offer the most noticeable benefits. This is because fasting helps tackle the core metabolic issues by lowering insulin levels and reducing hyperinsulinemia. In contrast, those with lean PCOS or ovulatory PCOS, where insulin resistance is less of a concern, may see fewer benefits. Research on fasting for these subtypes remains limited.
To help manage PCOS symptoms more effectively, Oana Health offers telehealth services that design personalized fasting plans tailored to your specific PCOS type, insulin resistance level, and overall health goals. These treatments are prescribed by licensed medical professionals and conveniently delivered right to your door.
